Claims management service model
We deliver a tailored experience by looking at the personal and physical needs of each claim, then select the right channel to help you manage and support you through the claim.
The icare claims management service model, introduced in January 2018, aims to achieve a better customer experience and better outcomes for employers and injured workers. Our model focuses on:
- simplicity
- consistency
- fairness
- transparency
- efficiency and
- financial sustainability.
The service model was designed to focus on the customer, to simplify the claims process and create increased transparency and effectiveness. It recognises the need for fast, efficient service for the majority of claims while ensuring claims at risk of prolonged time loss or with more complex circumstances receive the support they need.
We want to make the process simpler and faster, which is why we developed a segmented model that ensures appropriate levels of care and management are matched to the circumstances and complexities of the claim.
In September 2019, changes to how claims are managed in our Claims Support Centre came into effect. These changes apply to claim allocation rules which determine how claims are segmented and which claims go to which claims teams.
The adjustments changed how we manage medical only claims and claims where the worker is expected to take less than two weeks off work. The changes ensure that any claim with an expected incapacity likely to exceed two weeks will receive a dedicated case manager.
The customer experience
When lodging a claim, we ask several questions either of the employer or the injured worker. This helps direct the claim to the appropriate level of management, treatment and care.
If the claim is non-complex (for example, a medical only claim) we reduce the amount of intervention to deliver a faster resolution. We assign more complex claims to highly-trained, experienced case management specialists.
Throughout the claim lifecycle a number of flags and additional factors may indicate we need to investigate further, e.g. liability, requiring a change in case management support.
We aim to deliver the best return to work outcomes for injured workers and employers, appropriate to the claim. This model makes that a much more transparent and equitable process for all involved.
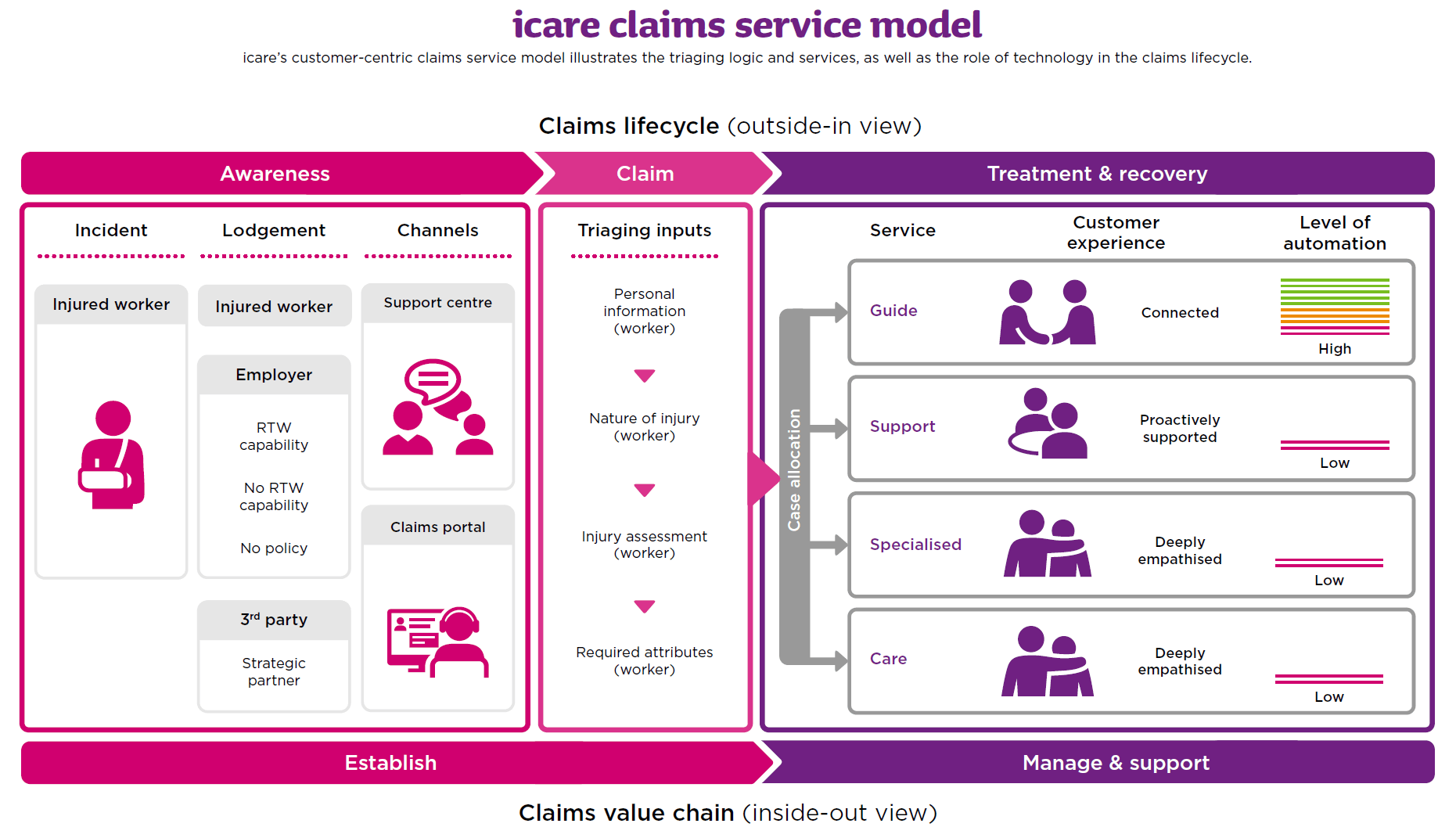
Workers Insurance claims lifecycle and value chain
Download this infographic
Claims management decision framework
The claims service model empowers claims service provider teams to be responsible for claims decisions to improve efficiencies and ensure that icare has visibility of dispute resolution and cost management to result in fairer outcomes for injured workers and employers.
As part of the implementation of icare’s service model, a claims management decision framework has been developed to better reflect the intent of the Workplace Injury Management 1987 and Workers Compensation Act 1998.
Claims management decision framework
Liability decisions
Core to the model is quickly directing claims to the right level of support and care. For instance, a simple, light-touch experience is where injured workers never take time off following injury. Simple, light touch instances make up 48 per cent of claims. Quickly directing this group of claims helps drive down year-on-year costs and handling expenses.
When a worker is injured on the job, and they’re unable to perform their pre-injury role we may accept provisional liability.
We've reduced the number of claims where we accept full liability at first decision, however the number of claims where we accept provisional liability has increased. This enables quicker time to treatment and more time to investigate before liability decisions are made.
Accepting provisional liability early, where appropriate, allows:
- the worker to get treatment faster
- leads to a quicker return to work
- reduces overall claim costs.
However, giving provisional liability does not mean we accept the claim. We perform a full liability assessment on all claims and involve the right people. We make the final liability decision in line with regulatory requirements.
Legislation guiding our decisions
Dispute resolution
Under icare’s Service Model, we play an active role in overseeing and managing disputes in their early stages. This allows us to resolve escalated disputes faster and give a better experience for both employers and workers.
We have a Dispute Resolution team in Personal Injury who is responsible for conducting internal reviews of liability and work capacity decisions made under icare’s Service Model by EML and Allianz when a request for an insurer review is made by the worker or employer.
The Dispute Resolution team is independent of the original decision and have decision making rights. They work closely with employers and workers to resolve disagreements about decisions made which affect a worker’s entitlement to benefits.
Types of workers insurance disputes
Medical Support Panel
Following a successful pilot in 2017, the Medical Support Panel (MSP) is now a permanent feature of icare’s customer-centric claims model.
Made up of doctors specialising in work injuries, the Panel provides case managers with:
- Medical advice and expertise to fast-track decision-making
- Support for both the injured worker and their employer.
By reviewing case information, the MSP medical specialists can make treatment and medical causation recommendations quickly, in an average of five days compared to six weeks before the commencement of the panel.

